Clinical Features and Treatment of Acute Patellar (Kneecap) Trauma: 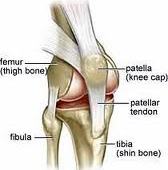
Acute trauma to the patella (e.g. from a hockey stick or from a fall onto the kneecap) can cause a range of injuries from fracture of the patella to osteochondral damage of the patellofemoral joint with persisting patellofemoral joint pain. In some athletes, the pain settles without any long-term sequelae. If there is suspicion of fracture, X-ray should be obtained. It is important to be able to differentiate between a fracture of the patella and a bipartite patella. A skyline view of the patella should be performed in addition to normal views. If there is no evidence of fracture, the patient can be assumed to be suffering acute patellofemoral inflammation. This can be a difficult condition to treat. Treatment consists of NSAIDs, local electrotherapy (e.g. interferential stimulation, TENS) and avoidance of aggravating activities such as squatting or walking down stairs. Taping of the patella may alter the mechanics of patellar tracking and therefore reduce the irritation and pain.
Fracture of the Patella
- Patellar fractures can occur either by direct trauma, in which case the surrounding retinaculum can be intact, or by indirect injury from quadriceps contraction, in which case the retinaculum and the vastus muscles are usually torn.
- Undisplaced fractures of the patella with normal continuity of the extensor mechanism can be managed conservatively, initially with an extension splint.
- Over the next weeks as the fracture unites, the range of flexion can be gradually increased and the quadriceps strengthened in the inner range.
- Fractures with significant displacement, where the extensor mechanism is not intact, require surgical treatment. This involves reduction of the patella and fixation, usually with a tension band wire technique.
- The vastus muscle on both sides also needs to be repaired. The rehabilitation following this procedure is as for undisplaced fracture.
Patella Dislocation
- Patella dislocation occurs when the patella moves out of its groove laterally onto the lateral femoral condyle.
- Acute patella dislocation may be either traumatic with a good history of trauma and development of a hemarthrosis following injury, or atraumatic, which usually occurs in young girls with associated ligamentous laxity, does not have a good history of trauma, and is accompanied by mild-to-moderate swelling.
Clinical Features
Patients with traumatic patella dislocation usually complain that, on twisting or jumping, the knee suddenly gave way with the development of severe pain. Often the patient will describe a feeling of something ‘popping out’. Swelling develops almost immediately. The dislocation usually reduces spontaneously with knee extension; however, in some cases this may require some assistance or regional anesthesia (e.g. femoral nerve block). A number of factors predispose to dislocation of the patella:
- Femoral anteversion
- Shallow femoral groove
- Genu valgum
- Loose medial retinaculum
- Tight lateral retinaculum
- Vastus medialis dysplasia
- Increased Q angle
- Patellar alta
- Excessive subtalar pronation
- Patellar dysplasia
- General hypermobility
The main differential diagnosis of patella dislocation is an ACL rupture. Both conditions have similar histories of twisting, an audible ‘pop’, a feeling of something ‘going out’ and subsequent development of hemarthrosis. On examination, there is usually a gross effusion marked tenderness over the medial border of the patella and a positive lateral apprehension test when attempts are made to push the patella in a lateral direction. Any attempt to contract the quadriceps muscle aggravates the pain. X-rays, including anteroposterior, lateral, skyline, and intercondylar views, should be performed to rule out osteochondral fracture or a loose body.
Treatment
- Treatment of traumatic patella dislocation depends on presentation. Relatively atraumatic dislocations are treated conservatively.
- Traumatic first- or second-time dislocations (hemarthrosis present) are treated with arthroscopic washout and debridement.
- Recurrent dislocation is treated with surgical stabilization.
- As a result, the rehabilitation program is lengthy and emphasizes core stability, pelvic positioning, vastus medialis obliquus strength, and stretching of the lateral structures when tight.
- The most helpful addition to patellofemoral rehabilitation in the recent past is increased emphasis on core stability.
- Similar to ACL intervention exercises, rotational control of the limb under the pelvis is critical to knee and kneecap stability.
Patella Fracture is common among athletes. It is an injury to kneecap. Major symptom of Patella Fracture is knee swelling. Alliance Rehab & Physical Therapy is the best Rehab & Physical Therapy center in Virginia. We provide 24/7 access to online appointments, with most of the requests scheduled in less than 48 hours.
Contact Us at: 703-751-1008